Realizing the benefits of MRI in the radiotherapy workflow
Despite MRI’s potential for radiotherapy, integrating the modality into the workflow can present challenges – specifically the novelty of a changed workflow and adjusting to the unique requirements for MRI use in radiation therapy versus as a diagnostic modality only .
Whether you are looking for a dedicated system in the RT department or for a shared service with radiology, Philips is committed to facilitating the integration of MRI and to helping you realize the benefits of MRI in radiation therapy.
Discover the benefits of MRI for radiotherapy
With its exceptional soft-tissue visualization capabilities and wide range of image contrasts, MRI has become a powerful tool to help more precisely define tumor boundaries. This is particularly important as it has been established that there is a high degree of uncertainty in target volume delineation, and it is even reported to represent the largest uncertainty in the entire radiotherapy process for most tumor sites**. Better visualization of the target area and nearby organs-at-risk is a key factor in enhancing target volume delineation. MRI’s expanding role also can be attributed to its functional imaging capabilities, which can inform both target characterization and treatment response.
- Excellent soft-tissue contrast
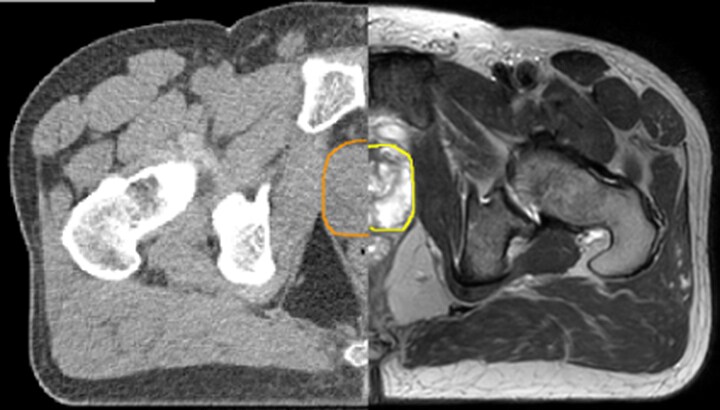
With its superior soft tissue contrast compared to CT, MRI offers exquisite visualization of tumor boundaries and proximity to nearby critical structures.
The ability to tune contrasts can provide even more valuable information about tumor characteristics and tumor extent to facilitate enhanced delineation, and also provides possibilities for dose boosting strategies. - Functional imaging
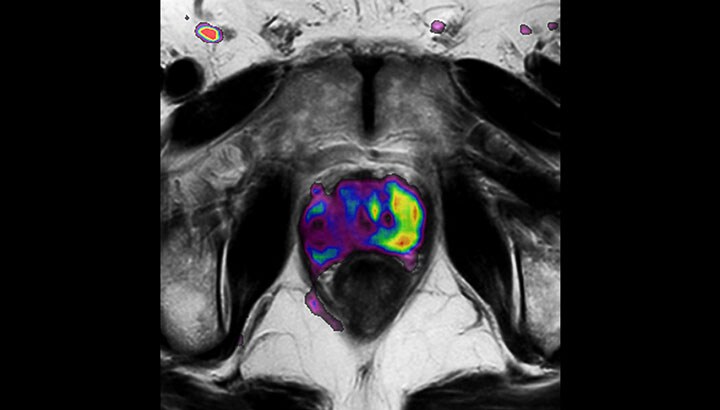
In addition to anatomical imaging, MRI offers the ability to obtain functional information that is beneficial for tumor detection and delineation, and for response monitoring.
Diffusion-weighted imaging (DWI) for example depicts areas of high signal intensity in soft tissues that are indicative of the restricted water mobility (i.e., diffusion) of a tumor and can also be used to identify lymph nodes. Changes in the tissue’s or lesion’s apparent diffusion coefficient (ADC) can provide insights that help predict the tumor’s response to radiotherapy. - No ionizing radiation
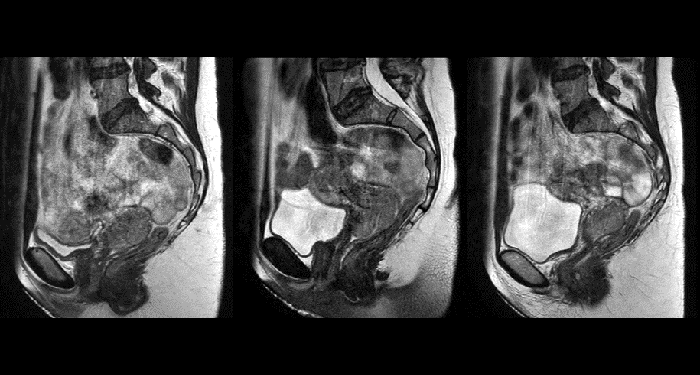
Unlike CT, MRI images are created without using ionizing radiation. This is particularly important when the patients are children, in which exposure to a radiation dose should be minimized to reduce long-term secondary effects. The option to acquire multiple MRI exams paves the road towards “plan-of-the-day” approaches or monitoring treatment response for adaptive strategies.
- Density information for dose calculation
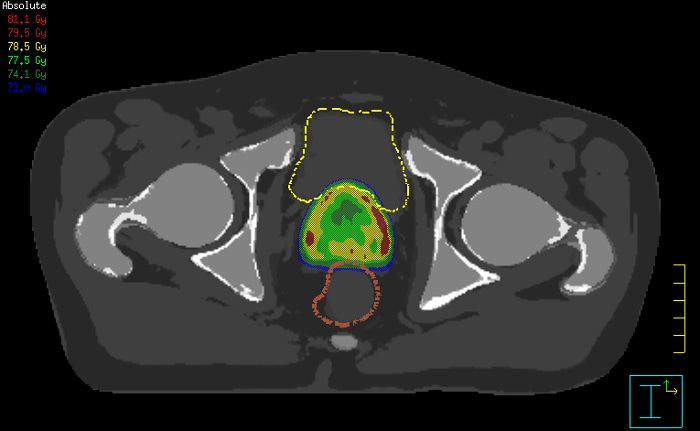
Innovative strategies in MRI-only simulation have made it possible to derive CT-like electron density information from MR imaging data. This capability enables physicians to use MRI as the radiotherapy department’s primary imaging modality for specific applications to eliminate tedious and error-prone CT-MR registration and simplify workflows.
